October 20, 2022
Member Spotlight: Hologic

Hologic Made Breast Cancer Screenings More Accurate with its 3D Mammography Imaging System and Works to Address Disparities in Healthcare for Women
Medical technology company Hologic was founded back in 1985, the same year that the American Cancer Society designated the month of October as National Breast Cancer Awareness Month. Since its founding, the company has grown to more than approximately 7,000 employees worldwide and is a leader in innovations for women’s healthcare. Hologic invented a mammography system that provides more accurate screenings for breast cancer, the digital breast tomosynthesis or 3D mammography imaging system, nearly a decade ago and continues to expand its diagnostic technologies. The company recently launched the multiyear Project Health Initiative pledging to provide breast cancer education, screenings and treatment for women in underserved communities, as well as an ambitious Global Women’s Health Index report. Hologic also debuted its first national campaign this year—including a commercial during the 2022 Superbowl with Grammy Award-winning singer Mary J. Blige—to raise awareness on the continued need for regular breast cancer screenings.
In celebration of Breast Cancer Awareness Month, we are featuring Erik Anderson, Hologic’s new division president for breast and skeletal health. He shares what makes Hologic’s technology different from standard mammograms, why the company is passionate about addressing inequities in healthcare, what role artificial intelligence and machine learning could play in advancing diagnostics and treatment for breast cancer, and why it’s important that companies continue making developments in diagnosing and treating the disease.
Hologic’s 3D mammography system is noted to help with earlier detection of breast cancer, is less invasive and works better for women with dense breast tissue—which 40 percent of women have. Can you summarize how 3D mammography works differently than traditional mammograms?
Hologic was the first company to receive FDA approval for 3D mammography imaging on our system just over 10 years ago. It has been a gamechanger for women’s screenings, especially those with dense breast tissue since our Genius exam is the only one that is FDA approved as superior to 2D mammography for women with dense breasts. i,ii
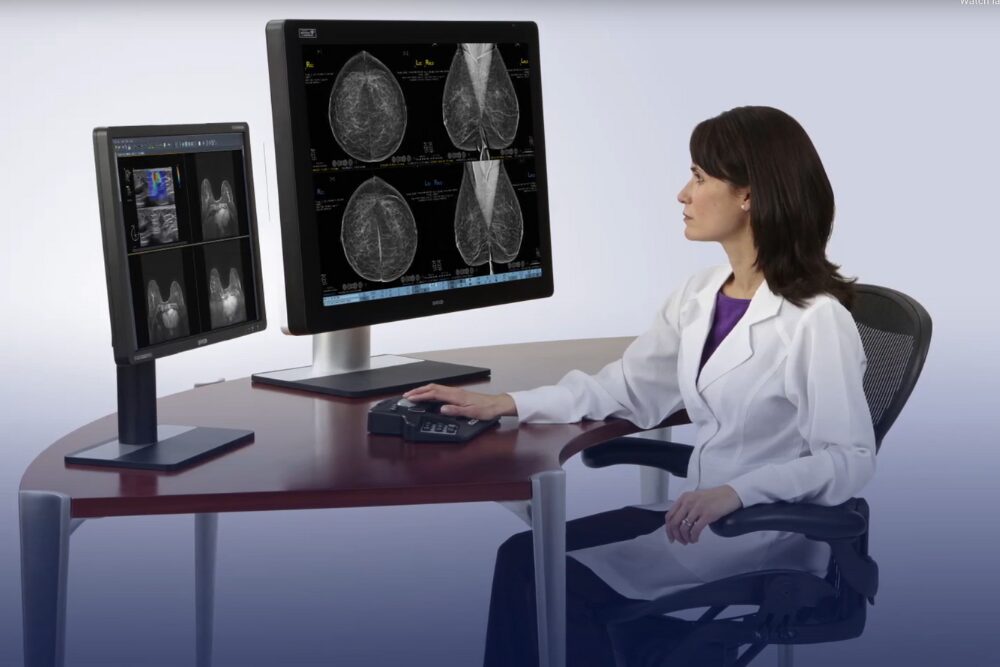
A traditional 2D mammogram consists of a single image of the breast, while 3D mammography captures multiple thin image “slices” of the breast tissue that allow the radiologist to see its different dimensions. When you capture a three-dimensional organ as a 2D image, layers of breast tissue can mask areas of concern that could eventually develop into cancer. However, with 3D imaging, the radiologist can assess breast tissue layer by layer, which can assist them in isolating lesions that might be hidden in dense breast tissue.
We know there is a need to continue generating awareness about breast cancer screening options and treatment … one of the most significant items we need to better understand is why women may not have access to this information or what prevents them from pursuing screening. There are several issues that still need to be overcome that create healthcare disparities.
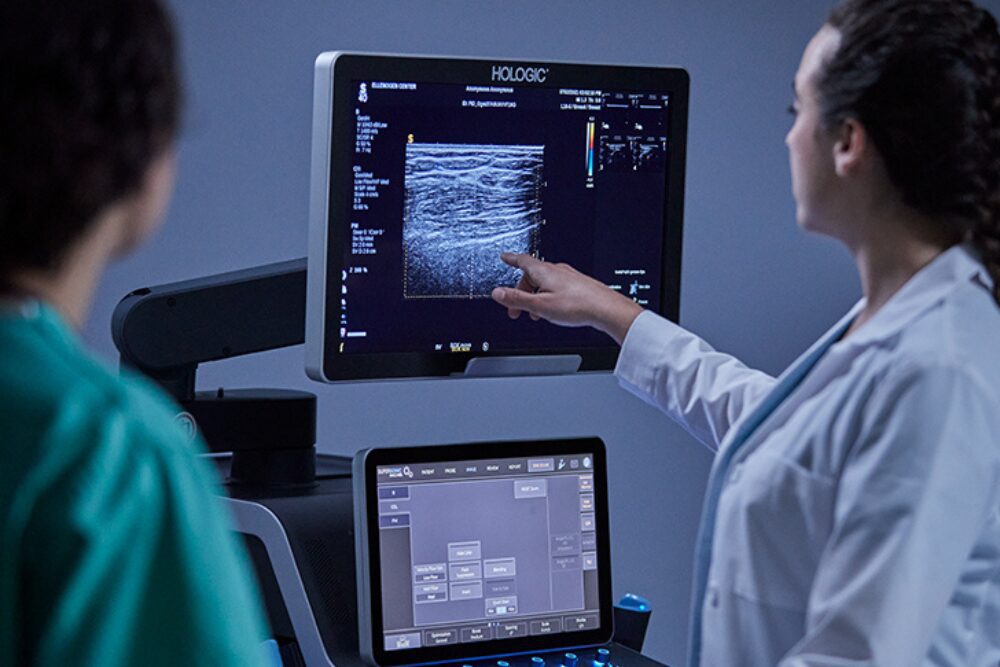
Is 3D mammography currently the standardized way to screen patients for breast cancer or must a patient search for a provider who is using it?
3D mammography is the gold standard for breast cancer screening. However, many patients still need to ask for it and there may not be a facility in their region offering the technology. The latest FDA data from March 2022 shows installation rates for digital breast tomosynthesis systems are rising. At the time, there were more than 10,700 digital breast tomosynthesis systems in service, representing about 45 percent of total U.S. mammography systems.i
One area that plays a key role in this discussion is healthcare disparities across the U.S. A 2021 study published in the Journal of the American College of Radiology found that Black women were less likely to receive screening via 3D mammography , even though research has shown that, despite having a similar breast cancer incidence rate, Black women are almost 40 percent more likely to die from breast cancer.ii
Inequitable access to 3D mammography technology is one reason why we launched our Project Health Equality (PHE) initiative in 2021, which is focused on helping to address health disparities faced by Black and Hispanic women through increased access to screenings and care, research, and education and awareness. By partnering with effective nonprofit organizations like the Black Women’s Health Imperative, National Alliance for Hispanic Health, and Promise Fund of Florida, we can help move the needle so more women are aware of the need for screenings and can access 3D mammography.
For women who would like to find a facility offering 3D mammography exams near them, they can utilize Genius3DNearMe.com
What is the biggest unmet health need for women today concerning breast cancer?
There are many unmet needs in breast health, with one of the biggest being inequitable access to screening technologies and the cost of care once a woman is diagnosed with breast cancer. We can continue to innovate equipment for better accuracy and fewer callbacks, but it does not mean anything if women are not being screened on systems that provide accurate data or cannot afford to be treated after diagnosis.
Ohio has become a shining example for breast cancer screenings, as the state has recently passed legislation that will require health insurance companies to cover the cost of additional imaging. But that only scratches the surface. Through Project Health Equality grants, we have been able to help our partner organizations through donations of 3D mammography systems and grants to fund patient navigator programs, where patients can work with a navigator to help them through their breast cancer journey.
This vital role helps patients overcome barriers that keep them from getting screenings and follow up care, such as arranging for transportation to appointments, providing translation services, and even helping them find funding programs for treatment.
Is there a new device in your product pipeline that will help address a current unmet diagnostics or treatment need? Is your breakthrough Genius AI Detection software in the works to be more widely available to help radiologists screen for breast cancer?
Artificial intelligence (AI) is a growing field in health care. Genius AI is our core AI technology, which builds on our 30-year history of innovation in breast health. We have several solutions powered by our Genius AI technology that integrate across the breast care continuum and that focus on aiding cancer detection, optimizing operational efficiency, and supporting clinical decisions.
Our latest breakthrough in deep learning-based cancer detection for breast tomosynthesis is Genius AI Detection technology, which launched in 2020 as part of our ongoing innovation to meet the needs of the breast health industry. This deep-learning technology helps radiologists prioritize cases and aids in their diagnostic performanceii by helping to detect subtle potential cancers in breast tomosynthesis images.
Innovations like AI will be the next gamechanger in breast health, and Hologic continues to explore how we can integrate this technology across systems so that it could one day not only identify a lesion, but also so much more, such as potentially provide quality control for biopsy procedures or identify cases that are almost certainly negative. The ultimate goal is to enable healthier lives, everywhere, every day—and we’re focusing our new technology innovations on delivering on that promise for the benefit of patients and physicians.
It’s known that breast cancer can be best treated when detected early through routine screenings. In Hologic’s studies and surveys, are you finding that women in the U.S. are not fully aware of the screening options that are available for them?
We recently completed a study that shows more women would like to know about breast cancer screening options earlier in their life, with many saying early teens would be the best time to begin discussions—right around when young adults are starting to learn about reproductive health. What was also interesting about this study was the lack of education about risk factors. For many of the women we surveyed, they did not know that there are in fact seven risk factors for breast cancer, including dense breast tissue, obesity, and family history.v
We know there is a need to continue generating awareness about breast cancer screening options and treatment, but in many ways one of the most significant items we need to better understand is why women may not have access to this information or what prevents them from pursuing screening. There are several issues that still need to be overcome that create healthcare disparities, including personal, financial, and language barriers to screenings and treatment, as well as the availability of equipment at facilities. Through Project Health Equality, Hologic is working to improve access in areas that are most affected.
A prime example of this is Found Care Palm Springs, a Federally Qualified Health Center in Palm Beach County, Florida, and the recipient of support from the Promise Fund. Before partnering with the Promise Fund, Found Care referred out for mammography services. For every 500 referrals, only about 100 received a mammogram. Today, more than 2,200 women have been screened at this facility, with more than a third for the first time, thanks in part to the donation of Hologic’s 3Dimensions mammography system that is now used at Found Care.
We know that 3D mammography detects non-invasive lesions sooner and reduces the number of call-backs up to 40 percent compared to 2D.ii,iii,iv Yet, many women are not receiving this standard of care.
What has been the biggest challenge for you to overcome in your career?
I am not different from anyone in that the pandemic has provided so many challenges to overcome. Millions of women were forced to cancel or reschedule their annual screenings due to facility closures or COVID-19 precautions. At the same time, our 350-plus field service team never left the front lines to take care of our caregivers in making sure their equipment was up to date and running to deliver patient care, uninterrupted. Our mission at Hologic is to empower women to live healthier lives. In the face of a pandemic, we needed to step up and support women by tackling their biggest health issues, in addition to providing solutions to help healthcare providers overcome screening backlogs and other COVID-19-induced challenges.
What is your biggest challenge at the moment?
I view personal and professional challenges as opportunities. As the new Division President for Breast and Skeletal Health, I have the opportunity to take on new responsibility and work with a broader team that shares the same mission and passion. The challenge with taking on a new leadership role is getting acclimated, but everyone in the division has come together to build upon the incredible foundation that is in place. I am truly honored to work with a team that helps continuously deliver on the high-quality medical technology Hologic has become known for in the breast health industry.
What does Breast Cancer Awareness Month mean to you, and why is it important that we recognize it?
The American Cancer Society (ACS) reported that breast cancer makes up 30 percent of all new cancer diagnoses among women each year, making it the second most common cancer for women. ACS also ranks breast cancer as the second leading cause of cancer deaths among women. We take an extraordinary amount of responsibility in driving the message home in recognizing Breast Cancer Awareness Month to build awareness about the preventative screening options available. When caught early, the five-year survival rate for breast cancer is close to 100 percent!iii,iv
What’s the greatest piece of advice you can give to future life science leaders?
Keep going—we have come a long way in the diagnosis and treatment of breast cancer, but there is more that needs to be done. Even in the most difficult moments, I reflect on the fact that what we do today saves lives, and the developments we make in the future will help save more. We can see a world where women are empowered to live healthy lives everywhere, every day—but we need the dedication of tomorrow’s leaders to make it happen.

i FDA submissions P080003, P080003/S001, P080003/S004, P080003/S005
ii Friedewald SM, Rafferty EA, Rose SL, et al. Breast cancer screening using tomosynthesis in combination with digital mammography. JAMA. 2014 Jun 25;311(24):2499-507.
iii https://radiologybusiness.com/topics/medical-imaging/womens-imaging/breast-imaging/3d-mammography-approaching-50-percent-breast
iv Alsheik, Nila et al. “Outcomes by Race in Breast Cancer Screening With Digital Breast Tomosynthesis Versus Digital Mammography.” Journal of the American College of Radiology : JACR vol. 18,7 (2021): 906-918. doi:10.1016/j.jacr.2020.12.033
v CDC, 2019. Health United States, 2018. Table 33
vi FDA Clearance K201109. * Based on analyses that do not control type I error and therefore cannot be generalized to specific comparisons outside this particular study. In this study: The average observed AUC was 0.825 (95% CI: 0.783, 0.867) with CAD and 0.794 (95% CI: 0.748, 0.840) without CAD. The difference in observed AUC was +0.031 (95% CI: 0.012, 0.051). The average observed reader sensitivity for cancer cases was 75.9% with CAD and 66.8% without CAD. The difference in observed sensitivity was +9.0% (99% CI: 6.0%, 12.1%). The average observed recall rate for non-cancer cases was 25.8% with CAD and 23.4% without CAD. The observed difference in negative recall rate was +2.4% (99% CI: 0.7%, 4.2%). The average observed case read-time was 52.0s with CAD and 46.3s without CAD. The observed difference in read-time was 5.7s (95% CI: 4.9s to 6.4s).
vii MISC-08197 MQD Consulting for Hologic, Mammography Patient Journey: Doorway Study, November 2021, U.S.
viii Rose S, Tidwell A, Bujnock L, et al. “Implementation of Breast Tomosynthesis in a Routine Screening Practice: An Observational Study.” American Journal of Roentengenology. 2013 Jun; 200(6): 1401-1408. Epub 2013 May 22.
ix Bernardi D, Macaskill P, Pellegrini M, et. al. Breast cancer screening with tomosynthesis (3D mammography) with acquired or synthetic 2D mammography compared with 2D mammography alone (STORM-2): a population-based prospective study. Lancet Oncol. 2016 Aug;17(8):1105-13
x National Breast Cancer Foundation, Inc. Stages 0 & 1: what does it mean to have stage 1 breast cancer? National Breast Cancer Foundation, Inc. Retrieved 3/31/15 from https://www.nationalbreastcancer.org/breast-cancer-facts.
xi Breastcancer.org. US breast cancer statistics. Breastcancer.org. https://www.breastcancer.org/symptoms/understand_bc/statistics. Retrieved 5/25/16.